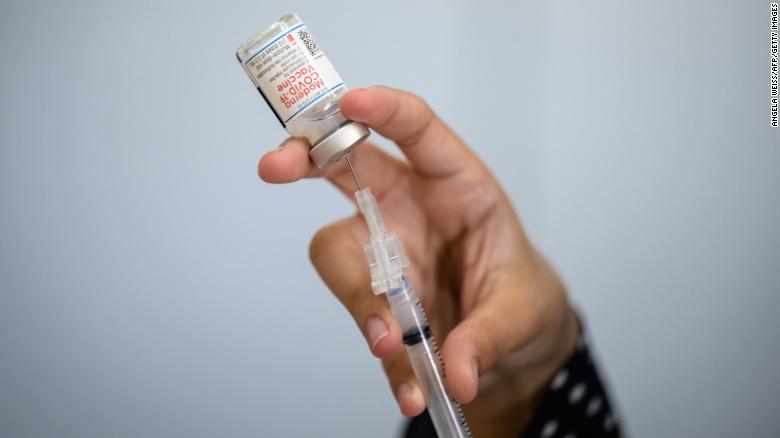
From Germany to the Dominican Republic, government health authorities are recommending the “mix-and-match” approach to vaccination in the hope of better protecting people by giving people them two different types of vaccine — one as a first dose, and another as a second or even a third dose.But does it really protect people better, and is it even necessary? From a scientific point of view, the jury is still out.Studies are currently underway to better understand the risks and benefits of mixing coronavirus vaccines — which might ease logistical problems for some global vaccine programs. But more research is needed to see whether mixed vaccine schedules work in the real world.

Germany issues world’s strongest recommendation for mixing Covid-19 vaccinesOn Thursday, Germany issued what appears to be the strongest recommendation anywhere for the mixing of coronavirus vaccines.The German Standing Committee on Vaccination (STIKO) said people who receive a first dose of the AstraZeneca vaccine “should get an mRNA vaccine as their second dose, regardless of their age.”The Pfizer/BioNTech and Moderna coronavirus vaccines use mRNA technology, while AstraZeneca’s vaccine uses a virus called an adenovirus to deliver immune-generating instructions to the body.STIKO said “current study results” show the immune response generated after a mixed dose vaccination “is clearly superior.”
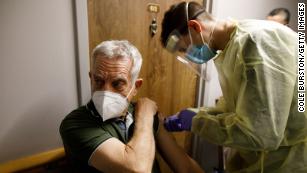
Mixing coronavirus vaccine brands is OK, Canada saysThe Dominican Republic said Thursday it would begin giving medical professionals a third, booster dose of vaccine to counter emerging coronavirus variants and said recipients should receive a different vaccine type from their first two doses. The country has been using three different vaccines: AstraZeneca’s, China’s Sinovac vaccine and the Pfizer/BioNTech vaccine.In June, Canada’s National Advisory Committee on Immunization made a weaker recommendation when it said “an mRNA vaccine is now preferred as the second dose for individuals who have received a first dose of AstraZeneca/COVISHIELD vaccine.”The Canadian committee said it was making the recommendation based on “emerging evidence of a potentially better immune response from this mixed vaccine schedule.”
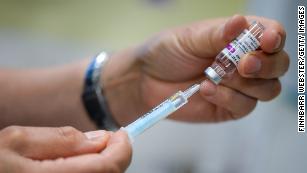
Mixing Covid-19 vaccines tied to more side effects, early UK data suggestsVaccine schedules that mix the Oxford/AstraZeneca and Pfizer Covid-19 vaccines all induced robust immune responses, although schedules including the Pfizer vaccine were stronger, researchers in the United Kingdom found.In a separate study, people who got mixed doses of coronavirus vaccines — receiving a different vaccine type as a second dose than the first dose — appeared to be more likely to experience mild side effects such as fever, chills, fatigue or headache, researchers in the UK reported in May in the Lancet medical journal.But the side effects following mix-and-match vaccinations were short-lived and there were no other safety concerns.
‘A research agenda to try and optimize vaccines’
The idea of using one type of vaccine for a first dose and a different type as the second has been exploredfor quite some time — even before the coronavirus pandemic, Dr. Amesh Adalja, senior scholar at the Johns Hopkins University Center for Health Security, told CNN on Friday. The concept is called heterologous prime-boost vaccination.”There were studies in the past with bird flu viruses using heterologous prime-boost, and this is part of a research agenda to try and optimize vaccines,” Adalja said.”It’s early in that research to understand where this will all end up several months to years from now in terms of what Covid vaccines will look like in the future. But it’s important to understand how to make better second-generation vaccines and to use this knowledge to even improve other vaccines for other infectious diseases,” Adalja added.
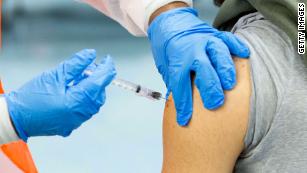
Organ transplant patients may benefit from third Covid-19 vaccine dose to boost antibodies, study suggestsIt’s important to understand how immune responses differ to different vaccines, Adalja said. The immune system responds in varying ways to different vaccine technologies.”This is a very fruitful area of research that’s important to understand, and it may help to design better vaccine regimens, especially in people that might not necessarily respond as well to the standard regimens — for example, an immunosuppressed person who’s had a solid organ transplant,” he said.One study, published in June in the journal Annals of Internal Medicine, suggests that a third dose of coronavirus vaccine could help boost antibody levels among some organ transplant recipients who have not had robust responses to the standard vaccination schedules.Among patients in the study who had no measurable antibodies after receiving two doses of vaccine, one-third saw a rise in antibodies after a third dose — and among those with low antibody levels after two doses, all of them saw an increase after a third dose. Some were boosted with the same vaccine but many were not.
Source:https://edition.cnn.com/2021/07/02/health/mixing-coronavirus-vaccines-explainer-wellness/index.html